Autoimmune Arthritis: Types, Symptoms, and Therapy
Understanding Autoimmune Arthritis
Autoimmune arthritis occurs when the immune system mistakenly attacks the body’s own joints, leading to inflammation, stiffness, and long-term joint changes. While symptoms vary by type, early recognition and proactive care can significantly impact daily mobility and long-term healthspan.
 Autoimmune arthritis is a chronic condition characterized by joint inflammation and pain caused by immune dysfunction.
Autoimmune arthritis is a chronic condition characterized by joint inflammation and pain caused by immune dysfunction.
Types of Autoimmune Arthritis
Identifying the specific type of arthritis is the first step in creating a targeted management plan:
- Rheumatoid Arthritis (RA): Targets the joint lining (synovium), typically affecting the hands, wrists, and feet symmetrically.
- Psoriatic Arthritis (PsA): Linked to psoriasis; often involves joint swelling, nail changes, and tendon inflammation.
- Ankylosing Spondylitis (AS): Primarily affects the spine and sacroiliac joints, leading to reduced flexibility.
- Lupus Arthritis: Joint pain that occurs as part of systemic lupus erythematosus (SLE).
- Reactive Arthritis: Inflammation that develops following certain bacterial infections.
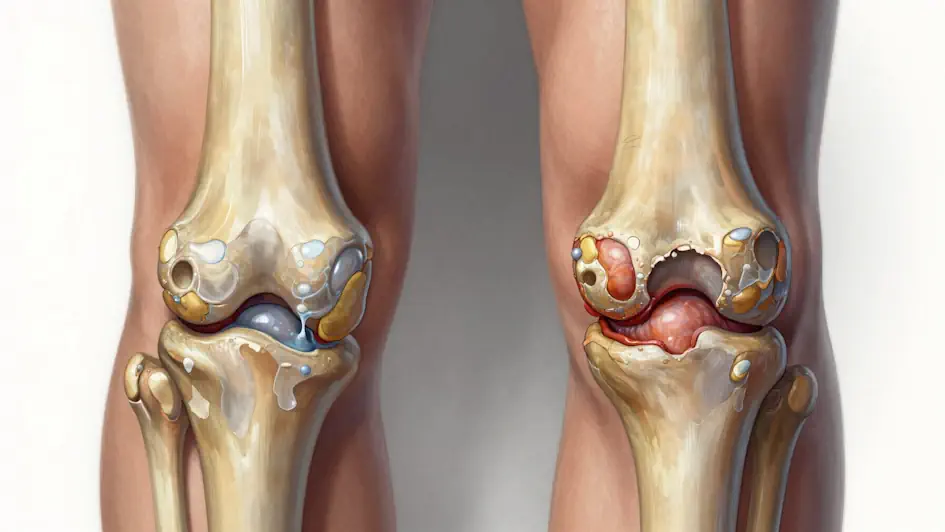 Figure 2: Left: A healthy knee with smooth cartilage and no inflammation. Right: A knee affected by rheumatoid arthritis, showing inflamed tissue, swollen synovium, and early joint damage.
Figure 2: Left: A healthy knee with smooth cartilage and no inflammation. Right: A knee affected by rheumatoid arthritis, showing inflamed tissue, swollen synovium, and early joint damage.
Common Symptoms and Warning Signs
Early detection is critical to preventing permanent joint damage. Watch for these persistent patterns:
- Morning Stiffness: Lasting longer than 30 minutes.
- Symmetrical Pain: Pain in the same joints on both sides of the body (common in RA).
- Systemic Fatigue: A profound sense of exhaustion that isn’t relieved by rest.
- Warmth or Redness: Joints that feel hot to the touch or appear swollen.
Management and Supportive Care
Treatment focuses on reducing systemic inflammation, protecting joint integrity, and supporting independent function.
Lifestyle and Movement:
- Gentle Movement: Low-impact activities like water exercise or stretching.
- Temperature Therapy: Using heat for morning stiffness and cold packs for acute swelling.
- Nutritional Support: Emphasizing whole foods to reduce inflammatory markers.
Supportive Therapies:
- Physical Therapy: Focuses on maintaining range of motion and muscle strength.
- Occupational Therapy: Provides strategies for “joint-friendly” daily tasks.
FAQ: Clinical Questions
Why does stress make my symptoms worse? Stress can increase the production of cortisol and inflammatory cytokines, which directly influences immune activity and flare-up intensity.
Is autoimmune arthritis the same as “wear-and-tear” arthritis? No. Osteoarthritis (wear-and-tear) is caused by mechanical breakdown, whereas autoimmune arthritis is caused by an overactive immune system.
Clinical Citations
- Arthritis Foundation: Arthritis Health Education A-Z
- NIAMS: Autoimmune Diseases Overview
- Mayo Clinic: Psoriatic Arthritis Symptoms