Psoriasis: Causes, Symptoms, and Treatments
Living Research: My 4-Year Psoriasis Journey
I don't just study psoriasis; I live it. For over four years, I have managed flare-ups primarily on my feet and legs. Recently, my journey took a turn as I began developing symptoms of Psoriatic Arthritis—a common but challenging progression where the immune system moves from the skin to the joints.
The Cost of Care: Two years ago, my insurance stopped covering Humira. Without AbbVie Assist (manufacturer patient assistance), I could not have afforded the biologic therapy that keeps my symptoms stable. This article combines my personal advocacy with the latest clinical data to help you navigate both the physical and financial hurdles of this condition.
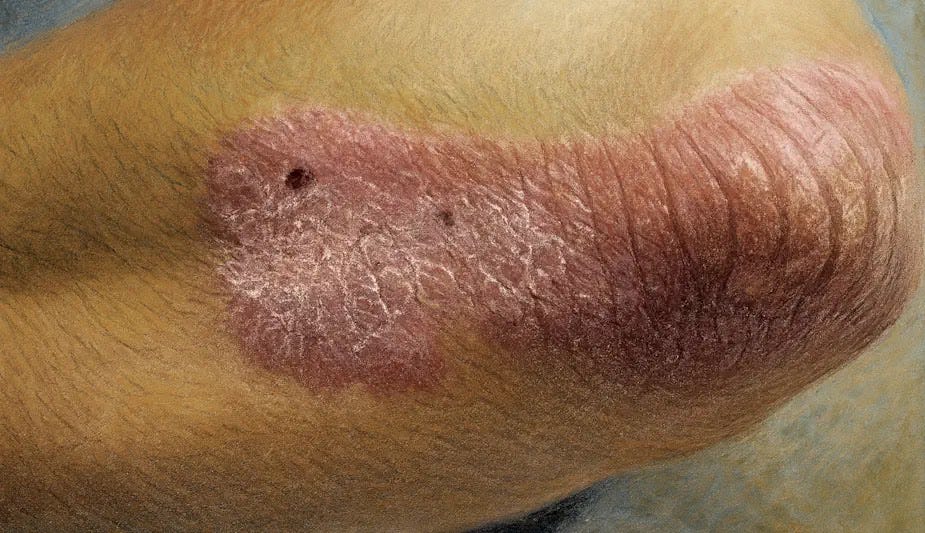
Psoriasis greatly impacts quality of life, requiring effective management and treatment. Early detection and intervention are essential. The visual effects of psoriasis highlight the need for timely treatment.
This article explores the many causes and wide range of symptoms linked to psoriasis, offering insight into the complexity of this chronic skin condition. By breaking down its details, it helps people better understand how psoriasis can affect both physical and emotional health.
It also covers different treatments and therapies, giving readers the knowledge they need to make informed choices about their care. By pointing out available resources and support networks, it encourages individuals to seek help and guidance in managing their condition.
Aiming to inspire people to take control of their health, this piece serves as a helpful guide for anyone wanting to live fully while dealing with the challenges of psoriasis.
What may cause or trigger psoriasis?
Causes or triggers of psoriasis can be varied. Psoriasis is marked by thick, scaly skin patches and doesn’t have one clear cause. Experts believe it develops due to a mix of genetic tendencies and environmental factors.
People with psoriasis have an overactive immune system that mistakenly attacks healthy skin cells. This speeds up skin cell growth, creating the plaques typical of the condition.
Genetics can make some people more likely to develop psoriasis, with certain genes increasing risk. Triggers like stress, infections, certain medications, and weather changes can worsen symptoms in those who are genetically prone, making this skin condition even more complex.
Is Psoriasis Hereditary?
Psoriasis can be linked to genetics, with over 80 genes tied to the condition. Still, carrying these genes doesn't guarantee it will appear. Environmental triggers play a big role in setting it off, even for those genetically predisposed.
This condition happens when the immune system overreacts to false alarms, leading to inflammation and rapid skin cell growth. Scientists are studying the specific genes involved, paving the way for new treatments like biologic therapies that focus on the immune system.
What are the main symptoms of psoriasis?
Psoriasis is a skin condition that impacts millions worldwide. It's a long-term autoimmune disorder where skin cells grow too fast, creating thick, red, and scaly patches. Several key symptoms can help spot this condition in people.
Psoriasis commonly presents as red, raised patches of skin covered with silvery scales, known as plaques, primarily found on elbows, knees, scalp, and lower back. These plaques can be itchy and painful and may crack or bleed if scratched.
Nail changes may occur, including discoloration, thickening, and pitting, with severe cases leading to separation from the nail bed (onycholysis).
Changes in eyebrows and eyelashes may include redness, scaling, and loss of eyelashes, impacting self-esteem and social interactions, but treatments are available to help manage these symptoms.
Scalp psoriasis is a long-lasting autoimmune disorder that causes the scalp to produce skin cells rapidly, resulting in red, itchy, and flaky patches. It affects about 50% of people with psoriasis, with genetic and immune system factors believed to contribute to its development.
Beyond physical symptoms, psoriasis can significantly impact emotional health, leading to feelings of embarrassment, low self-esteem, and social withdrawal, which may result in anxiety and depression, ultimately diminishing a person's quality of life.
While there is no cure for psoriasis, there are several treatment options available to help manage the symptoms and improve quality of life. These may include topical creams and ointments, oral medications, phototherapy, and biologic injections. It is important for individuals with psoriasis to work closely with their healthcare provider to find a treatment plan that works best for them.
When Skin Meets Bone: Psoriatic Arthritis (PsA)
About 30% of people with psoriasis will develop Psoriatic Arthritis. In my experience, it starts as a subtle stiffness. Clinical signs include:
Dactylitis: "Sausage-like" swelling of fingers or toes.
Enthesitis: Pain where tendons meet bone (common in the heels or elbows).
Morning Stiffness: Joint pain that takes 30+ minutes to "warm up" after waking.
Researcher's Tip: Early intervention with biologics is key to preventing permanent joint damage. Don't ignore "minor" joint aches if you have active skin plaques.
Navigating the Biologic "Paywall"
Biologics like Humira, Skyrizi, and Cosentyx are life-changing but can cost $5,000+ per month. When my insurance pulled coverage, I learned that the system is negotiable.
Resource What it Does Who it’s For Patient Assistance Programs (PAP) Programs like AbbVie Assist provide medication for $0 to low-income/uninsured patients. Uninsured or under-insured patients. Copay Cards Manufacturer cards that lower your pharmacy out-of-pocket to as little as $5. Patients with commercial insurance. Step Therapy The "Fail First" rule where insurance makes you try cheaper drugs before biologics. A common hurdle for new diagnoses.
Managing systemic inflammation is similar to how I approach Liver Cirrhosis and heart health—it's all about reducing the internal fire.
What are the different types of psoriasis?
1. Plaque psoriasis
Plaque psoriasis is the most common form of this long-term skin condition, affecting about 80% of those who have psoriasis. It's marked by red, raised patches of skin covered with silvery scales, making it the most recognizable type of psoriasis.
These plaques often appear on noticeable areas like the elbows, knees, scalp, and lower back, reflecting the inflammation happening beneath the skin's surface. The rapid growth of skin cells causes these patches, which can be itchy, uncomfortable, and take a toll on daily life.
Knowing what plaque psoriasis looks like and how it impacts people is key to managing symptoms and improving overall quality of life.
2. Guttate psoriasis
Guttate psoriasis is an autoimmune skin condition characterized by small, red, scaly spots that look like teardrops.
These lesions can appear on the arms, legs, and torso, often triggered by bacterial infections, especially streptococcal throat infections.
It is more common in children and young adults and can be confused with other skin problems like eczema or fungal infections.
Early diagnosis and treatment are essential for managing symptoms and preventing flare-ups.
Dermatologists may recommend topical treatments, phototherapy, or systemic medications to improve symptoms and quality of life.
3. Inverse psoriasis
Inverse psoriasis is a type of psoriasis that typically develops in skin folds, such as the armpits, groin, or beneath the breasts. Unlike the more common form, which produces scaly patches on areas like the elbows, knees, and scalp, inverse psoriasis presents as smooth, red, and shiny lesions.
These affected areas are prone to sweating and friction, which can lead to irritation, discomfort, and potential infection. Individuals with inverse psoriasis may experience pain and itching that interfere with daily activities.
Accurate diagnosis and appropriate treatment are essential for managing symptoms and enhancing quality of life.
4. Pustular psoriasis
Pustular psoriasis is a rare type of psoriasis marked by white pustules surrounded by red skin. It often appears on specific areas like the palms and soles but can spread more widely. The pustules are filled with non-infectious white blood cells, tend to be tender, and contain pus.
People with this condition may also have symptoms like fever, chills, severe itching, and fatigue. Because it can be serious and sometimes widespread, it can greatly affect quality of life and often needs specialized medical care.
Getting advice from healthcare professionals is important for proper diagnosis and personalized treatment.
5. Erythrodermic psoriasis
Erythrodermic psoriasis is a rare, severe form of psoriasis that affects the entire body, marked by widespread redness, inflammation, and skin exfoliation. This condition can be profoundly debilitating, with patients experiencing intense itching, pain, and discomfort, alongside significant impacts on quality of life. The emotional and psychological burden is considerable and should not be overlooked.
What are some psoriasis treatments?
While there's no cure for psoriasis, there are plenty of treatments that can help manage symptoms and improve the look and feel of your skin. These options work to reduce inflammation, slow skin cell growth, and ease discomfort.
Common treatments include topical creams, light therapy, oral medications, and biologic injections. It's important to work with a healthcare provider to create a treatment plan that fits your needs and helps you manage the condition over time.
Living with psoriasis can be tough, as it often affects both daily routines and emotional well-being. You're not alone-millions of people deal with it every day. There are many resources and support networks available to help you manage the condition, both physically and emotionally.
By connecting with others who understand and leaning on support systems, you can build resilience and maintain a good quality of life despite the challenges psoriasis may bring.
How to cope living with psoriasis
Living with psoriasis can be tough, as it often affects both daily routines and emotional well-being. You're not alone-millions of people deal with it every day. There are many resources and support networks available to help you manage the condition, both physically and emotionally. By connecting with others who understand and leaning on support systems, you can build resilience and maintain a good quality of life despite the challenges psoriasis may bring.
Here are a few tips for living with psoriasis:
Find a doctor specializing in psoriasis: A dermatologist can help you develop a treatment plan.
Increased knowledge concerning psoriasis will help to manage your condition.
Join a support group for people with psoriasis. Joining a support group can help you connect with other people who understand what you are going through.
Take care of your skin: Moisturizing your skin often to reduce dryness and itching. Avoid harsh soaps and detergents, and take warm baths and showers instead of hot baths and showers.
Manage your stress: Stress can trigger psoriasis flare-ups. Find healthy ways to manage stress, such as exercise, relaxation techniques, and spending time with loved ones.
How Nightshade Foods May Agitate Psoriasis Symptoms
Nightshades are fruits, vegetables, and herbs from the Solanaceae family. Common examples include tomatoes, bell peppers, potatoes, and eggplant.
Toxic Molecules
Nightshades produce alkaloids, natural defense chemicals that can irritate the gut or immune system in sensitive individuals. There is no scientific consensus that nightshades worsen psoriasis, but some people report increased irritation or inflammation.
In a 2017 National Psoriasis Foundation survey, 52.1% of respondents said removing nightshades improved their skin. Results vary from person to person.
Nightshade Vegetables
Tomatoes: Used in salads, sauces, and many dishes.
Potatoes: Regular potatoes (not sweet potatoes).
Eggplant: Common in Mediterranean and Middle Eastern cuisine.
Peppers: Includes hot and sweet peppers; paprika and chili powder come from these.
Note: These may cause issues for those sensitive to nightshades.
Nightshade Fruits
Goji berries: Often marketed for antioxidants.
Tomatillos: Used in Mexican cuisine.
Pepino: Mild, sweet “melon pear.”
Ground cherries: Used in jams and desserts.
If you have sensitivities or allergies, these may be worth avoiding.
Nightshade Spices
Paprika: Sweet and smoky flavor.
Cayenne pepper: Hot, spicy ground pepper.
Red pepper flakes: Crushed chili peppers.
Chili powder: Blend of chili peppers and spices.
If you experience any adverse reactions, consult a healthcare professional.
Real-Life Case Study
Maria, a 42-year-old teacher, noticed persistent scaling on her elbows and knees. After months of discomfort and misdiagnosis, she was finally diagnosed with plaque psoriasis. With a tailored treatment plan, she regained confidence and control over her symptoms.
Treatment Options in 2024 and Beyond
Topical Treatments
Corticosteroids: Reduce inflammation and slow skin turnover.
Vitamin D analogs: Help normalize skin cell growth.
Calcineurin inhibitors: Suppress immune activity in sensitive areas.
Phototherapy
UVB light therapy: Can slow skin cell growth and reduce inflammation.
Systemic Medications
Oral drugs: Methotrexate, cyclosporine.
Biologics: Target specific immune pathways (e.g., IL‑23 inhibitors).
Recent advances include steroid‑free topicals and smartphone‑powered light treatments.
Lifestyle and Complementary Therapies
Anti‑inflammatory diets
Stress management
Moisturizing routines
Glossary
Biologics
Advanced medications that target specific parts of the immune system.
Interleukin‑23 (IL‑23)
A protein involved in inflammation, targeted by newer biologics.
Phototherapy
Treatment using ultraviolet light.
Psoriatic Arthritis
A form of arthritis affecting some people with psoriasis.
Calcineurin Inhibitors
Topical drugs that suppress immune activity.
Hyperproliferation
Excessive cell growth, common in psoriasis.
Drug Class Common Examples How it Works Focus Area TNF Inhibitors Humira, Enbrel, Remicade Blocks Tumor Necrosis Factor (a broad inflammatory protein). Gold Standard for both skin and joint stiffness. IL‑17 Inhibitors Taltz, Cosentyx Targets the specific IL‑17 protein that drives plaque growth. High success rate for rapid skin clearance. IL‑23 Inhibitors Skyrizi, Tremfya Targets the “upstream” signal of inflammation. Known for long‑lasting results and fewer doses. JAK Inhibitors Xeljanz, Rinvoq (Oral pills) Blocks the “switches” inside immune cells. Great for those with needle phobia or who fail injections.
FAQs
Q1: Is psoriasis curable?
A: No, but it is manageable with the right treatment plan.
Q2: Can diet affect psoriasis?
A: Anti-inflammatory diets may help reduce flare-ups.
Q3: What's the difference between eczema and psoriasis?
A: Psoriasis has thicker scales and is immune-mediated, while eczema is more allergy-related.
Q4: Are biologics safe?
A: Generally, yes, but they require monitoring for side effects.
Q5: Can children get psoriasis?
A: Yes, though it's less common. Pediatric treatment options are available.
Conclusion
Psoriasis is a lifelong condition, but with the right knowledge and support, patients can manage symptoms and improve their quality of life. This guide offers a foundation for better healthcare conversations, helping patients advocate for themselves with clarity and confidence.
Toggle References
Dermatology Times: Psoriasis Therapies in 2024 and Beyond【1】
National Library of Medicine: Challenges and Future Trends in Psoriasis Treatment【2】
Healthline: New Psoriasis Treatments in 2024【3】
WebMD: Advances in Psoriasis Treatments【4】
Verywell Health: Managing Psoriasis Flares【5】
National Psoriasis Foundation: American Academy of Dermatology: Mayo Clinic: Nightshades and Psoriasis Psoriasis_on_back.jpg: User: The Wednesday Island derivative work: James Heilman, MD, Mohammad2018,
Disclaimer:
I am not a medical professional. The information provided on this blog is for informational purposes only. It is not a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified healthcare provider with any questions you may have regarding a medical condition.


