Liver Cirrhosis - What You Need to Know
Liver Cirrhosis: Understanding the Causes, Symptoms, and Treatment Options
Managing decompensated liver cirrhosis is a full-time job for both the body and the mind. For seniors and caregivers, the "So-What" is moving from a state of crisis to a state of stabilized management. By understanding the mechanics of portal hypertension and the necessity of repeated banding, patients can reduce medical anxiety and focus on quality of life, even when a transplant is not the immediate goal.
Medical Disclaimer: This content is for informational and educational purposes only. It does not replace professional medical advice, diagnosis, or treatment. Always consult a qualified healthcare provider regarding any medical condition.
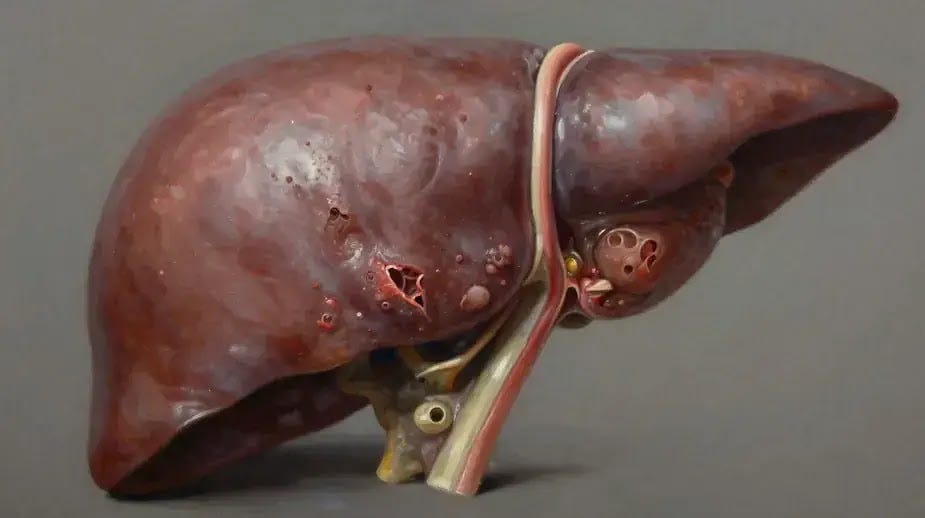
Cirrhosis is the advanced stage of liver disease, characterized by severe, irreversible liver damage as healthy tissue is replaced by scar tissue, impairing liver function.
Liver Cirrhosis: A Clinical and Personal Guide to Decompensation
Liver cirrhosis is the final common pathway of chronic liver injury. Whether caused by alcohol, viral hepatitis, or MASLD (fatty liver), the result is the same: healthy tissue is replaced by fibrotic scarring that distorts blood flow.
Liver Cirrhosis: A Clinical and Personal Guide to Decompensation
Liver cirrhosis is the final common pathway of chronic liver injury. Whether caused by alcohol, viral hepatitis, or MASLD (fatty liver), the result is the same: healthy tissue is replaced by fibrotic scarring that distorts blood flow.
The Tipping Point: Compensated vs. Decompensated
Compensated: The liver is scarred but still performing its primary functions. This stage can be "silent" for years.
Decompensated: This is marked by the onset of overt complications like ascites (fluid), jaundice (yellowing), or variceal bleeding.
As a patient living with decompensated cirrhosis, I have learned that "decompensation" isn't a single event—it is a shift into a new phase of life that requires constant vigilance and specialized care.
Portal Hypertension: The Root of the Complications
As scar tissue blocks the flow of blood through the liver, pressure builds in the portal venous system. To compensate, the body reroutes blood through smaller, fragile vessels.
Esophageal Varices: These are "pressure relief valves" in the throat. Because they are thin-walled, high pressure can cause them to burst.
The Role of Banding (EVL): Endoscopic variceal band ligation is not a "one and done" fix. As I have experienced through more than ten procedures, repeated banding is a preventative strategy to keep these vessels from rupturing. It is not a sign of treatment failure; it is active maintenance.
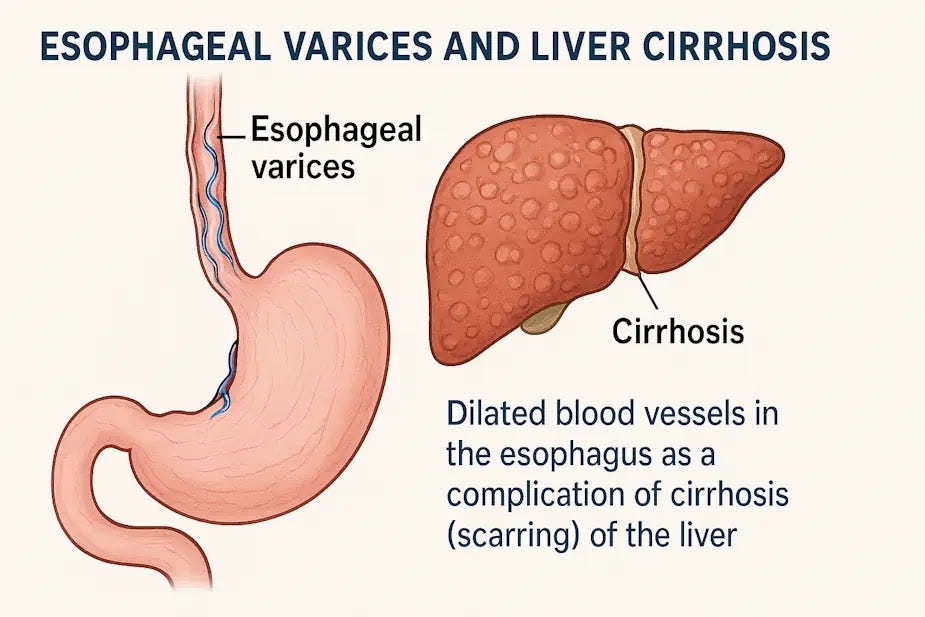
Dilated veins in the esophagus (varices) develop when cirrhosis increases pressure in the portal vein system. These fragile veins can rupture and cause life‑threatening bleeding, making regular monitoring essential for people with advanced liver disease.
Beyond the Liver: The Systemic Impact
Cirrhosis affects the entire biological ecosystem.
Anemia and Breathlessness: A damaged liver produces fewer proteins and clotting factors. Chronic anemia means your blood carries less oxygen. On days when I struggle to catch my breath, it is a reminder that cirrhosis is a systemic condition.
Hepatic Encephalopathy (HE): When the liver fails to filter toxins like ammonia, they reach the brain. Consistent use of lactulose and rifaximin is the "Gold Standard" for preventing the confusion and cognitive decline associated with HE.
Treatment: What Actually Helps?
According to the American Association for the Study of Liver Diseases (AASLD), individualized care is paramount:
Beta-Blockers (e.g., Carvedilol): Used to lower the internal pressure and prevent the need for frequent banding.
Albumin Therapy: Recent research suggests long-term albumin can stabilize patients with recurrent ascites.
Transplant Evaluation: The new AASLD/AST guidelines advocate for earlier referral, often as soon as the first decompensation event occurs.
FAQ: Understanding Advanced Liver Disease
1. Why do I need repeated variceal banding?
Banding treats the symptom (the varices), not the cause (the pressure). Until the portal hypertension is managed, new varices will likely form.
2. Can I live a full life with decompensated cirrhosis?
Yes. Stabilization through medication adherence and regular surveillance (endoscopy every 6–12 months) allows many patients to live for years post-diagnosis.
3. What does a rising MELD score mean?
The MELD (Model for End-Stage Liver Disease) score predicts short-term mortality risk. It is used to prioritize transplant candidates, but it doesn't always reflect how you "feel" daily.
📘 POST‑LEVEL MINI GLOSSARY
Hepatic Encephalopathy
A brain‑related complication of liver disease caused by a buildup of toxins—especially ammonia—that the liver can no longer clear. It can cause confusion, sleep changes, irritability, or slowed thinking.
Albumin
A protein made by the liver that helps maintain fluid balance in the bloodstream. Low albumin can lead to swelling, fatigue, and fluid buildup.
Albumin Therapy
An IV treatment used to restore albumin levels. It helps stabilize blood pressure, reduce fluid overload, and support kidney function during complications like large‑volume paracentesis or infections.
Esophageal Varices
Enlarged veins in the esophagus caused by portal hypertension. These veins can rupture and bleed, making regular monitoring essential.
Banding (Variceal Band Ligation)
A procedure where rubber bands are placed around varices to stop bleeding or prevent future bleeding. It treats the veins, not the underlying pressure.
Beta‑Blockers
Medications that lower portal pressure and reduce the risk of variceal bleeding. Common examples include propranolol and nadolol.
Compensated Cirrhosis
Cirrhosis where the liver is scarred but still performing enough essential functions to avoid major complications.
Decompensated Cirrhosis
Advanced cirrhosis where the liver can no longer keep up. Complications such as ascites, variceal bleeding, jaundice, or encephalopathy may occur.
💡 The Liver-Brain Connection
It is important to remember that metabolic health isn't localized. Research into Type 3 Diabetes shows that the same insulin resistance that complicates liver recovery can also lead to neuroinflammation. To see how I am connecting these dots, read my latest research on Is Alzheimer’s Really Type 3 Diabetes?
Professional Sources & Scholarly References
AASLD Practice Guidelines: Adult Liver Transplantation: Diagnosis and Management.
Liver Fellow Network: ACLF: The Tipping Point in Chronic Liver Disease.
Clinical Trials Research: The role of long-term albumin therapy in treating decompensated cirrhosis.


