Edema: Information about Causes and Effective Treatments
Understanding Edema: Causes Symptoms and Solutions
Due to my liver cirrhosis, I experience recurring edema. At times, the swelling becomes severe enough that the skin feels tight and causes aching pain in my legs. To manage this, I wear compression/support stockings daily. I am also required by my doctor to elevate my feet above hip level for one hour for every two hours that I am standing, as prolonged standing significantly worsens the swelling and discomfort.
Medical Disclaimer: This content is for informational and educational purposes only. It does not replace professional medical advice, diagnosis, or treatment. Always consult a qualified healthcare provider regarding any medical condition.
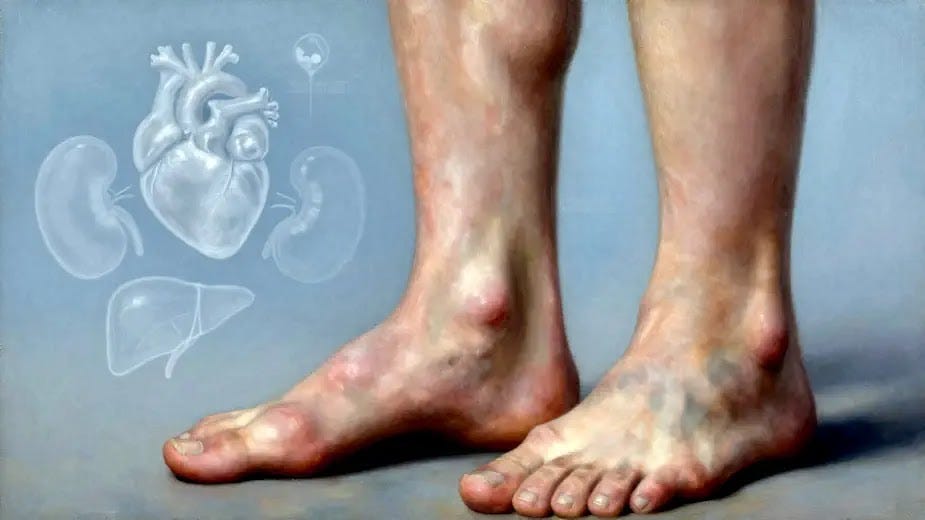
The swollen legs and ankles highlight the visible impact of edema. Some of the underlying causes are heart failure, kidney disease, cirrhosis, and drug side effects.
Key Points at a Glance
Edema is swelling caused by excess fluid trapped in body tissues. It most commonly affects the legs, ankles, feet, hands, and face.
Causes range from temporary lifestyle factors to serious underlying medical conditions.
Treatment depends on identifying the root cause, not just reducing swelling.
Persistent, painful, or sudden edema requires medical evaluation.
What Is Edema?
Edema is a medical condition characterized by the abnormal accumulation of fluid in the interstitial spaces of tissues. While mild edema can be harmless and temporary, chronic or sudden-onset edema may signal problems involving the **heart, kidneys, liver, lymphatic system, or blood vessels.
Edema can be localized (affecting one area) or generalized (affecting the whole body).
1. Common Causes of Edema.
Lifestyle and Environmental Causes
Prolonged sitting or standing
High sodium (salt) intake
Pregnancy-related fluid retention
Hot weather
Long-distance travel (e.g., flights)
2. Medical Conditions
Heart failure: Reduced pumping efficiency leads to fluid buildup
Kidney disease: Impaired fluid excretion
Liver disease (cirrhosis): Low albumin levels cause fluid leakage
Chronic venous insufficiency: Poor blood return from legs
Lymphedema: Lymphatic system blockage
Deep vein thrombosis (DVT): Blood clot causing unilateral swelling
3. Medications Linked to Edema
Calcium channel blockers
NSAIDs (e.g., ibuprofen)
Corticosteroids
Hormonal therapies (estrogen, testosterone)
Symptoms of Edema Common signs include:
Visible swelling or puffiness
Skin that appears shiny or stretched
Pitting edema (indent remains after pressing skin)
Tightness or heaviness in limbs
Reduced joint flexibility
Rapid weight gain from fluid retention
Red-Flag Symptoms (Seek Immediate Care)
Sudden swelling in one leg
Chest pain or shortness of breath
Swelling accompanied by fever or redness
Facial swelling with difficulty breathing
Decision Tree: When to Worry About Edema
Is the swelling mild and temporary?
│
├── Yes → Recent standing, travel, salt intake?
│ └── Yes → Lifestyle-related edema → Monitor & adjust habits
│
└── No
│
├── Is swelling persistent (>1–2 weeks)?
│ └── Yes → Medical evaluation recommended
│
├── Is it one-sided, painful, or sudden?
│ └── Yes → Possible DVT → Seek urgent care
│
└── Is swelling with shortness of breath or chest pain?
└── Yes → Emergency → Call emergency services
Diagnosis of Edema Healthcare providers may use:
Physical examination (pitting test)
Blood tests (kidney, liver, heart markers)
Urine analysis
Ultrasound or Doppler studies
Echocardiogram (if heart-related cause suspected) -
Treatment and Solutions for Edema
Lifestyle & Home Remedies
Reduce sodium intake
Elevate affected limbs
Wear compression stockings
Maintain healthy body weight
Stay physically active
Medical Treatments
Diuretics (fluid-reducing medications)
Treating underlying conditions (heart, kidney, liver disease)
Manual lymphatic drainage therapy
Medication adjustment or substitution
Important: Never start or stop medications without consulting a healthcare professional.
Seniors Want to Know
Swelling in Lower Legs (No Pain)
Venous insufficiency causing fluid pooling
Long sitting or standing periods
High sodium intake
Medication effects (BP meds, steroids, hormones)
Heart, kidney, or liver conditions
Obesity increasing vein pressure
Early lymphedema (often painless)
New or one‑sided swelling should be evaluated.
Non‑Pitting Edema
Swelling that does not leave an indentation when pressed
Usually protein‑rich fluid, not just water
Common causes: lymphedema, thyroid issues, lymphatic damage
Often needs clinical evaluation.
Edema vs. Lymphedema
Edema: Often pitting, soft, linked to salt, gravity, or organ issues
Lymphedema: Often non‑pitting, firm, chronic, lymphatic blockage
Lymphedema may cause skin thickening over time
Lymphedema is typically long‑term and progressive.
Fluid Retention in Ankles
High sodium intake
Heat exposure
Prolonged sitting or standing
Venous insufficiency
Medications (BP meds, NSAIDs, steroids)
Heart, kidney, or liver conditions
Obesity or pregnancy
Sudden or one‑sided swelling warrants prompt evaluation.
Frequently Asked Questions (FAQ)
Can edema go away on its own?
Yes, mild edema caused by lifestyle factors often resolves with rest, elevation, and dietary changes.
Is edema always a sign of heart failure?
No. While heart failure can cause edema, many cases are due to benign or temporary causes.
What’s the difference between edema and lymphedema?
Edema is general fluid buildup, while lymphedema involves lymphatic system dysfunction and often requires specialized treatment.
Can dehydration cause edema?
Paradoxically, yes. Severe dehydration can trigger the body to retain fluid.
When should I see a doctor for swelling?
If edema is persistent, painful, sudden, or associated with breathing issues, seek medical care promptly.
📘 Related Patient Resources
The Log: Start tracking your “Mental Clarity” score with my Daily Glucose Tracker.
The Foundation: New to this? Read my Beginner’s Guide to Diabetes.
Liver Health: How metabolic syndrome impacts liver cirrhosis .


