Physical Therapy - Benefits Autoimmune Arthritis Patients
Autoimmune Arthritis Relief: The Role of Physical Therapy
Physical therapy is crucial for managing autoimmune arthritis, improving mobility and reducing symptoms. Customized exercises help patients regain strength, flexibility, and range of motion, empowering them to manage their condition and enhance their quality of life.
Medical Disclaimer: This content is for informational and educational purposes only. It does not replace professional medical advice, diagnosis, or treatment. Always consult a qualified healthcare provider regarding any medical condition.
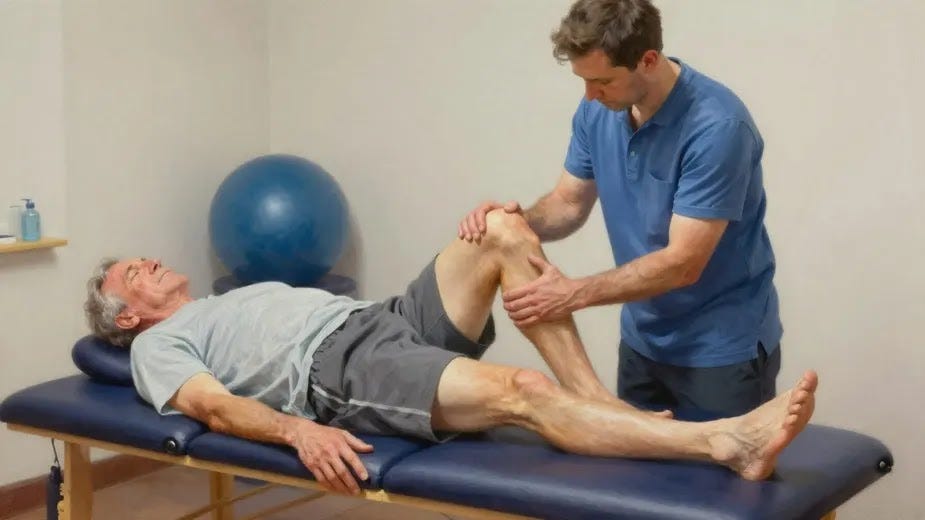
Physical therapy offers a multitude of advantages for individuals suffering from autoimmune arthritis, a condition characterized by inflammation and pain in the joints due to the immune system mistakenly attacking healthy tissues.
Understanding the Impact of Autoimmune Arthritis
Autoimmune arthritis includes conditions such as rheumatoid arthritis, psoriatic arthritis, and axial spondyloarthritis . are characterized by the immune system erroneously targeting and damaging the body's own tissues. Regular, moderate exercise has immunomodulatory effects and is associated with reduced systemic inflammation over time.
Physical Therapy Helps Mobility, Strength, and Flexibility.
You and Your Healthcare Team
By partnering with a physical therapist, people living with autoimmune arthritis can take an active role in managing symptoms, restoring function, and improving daily quality of life. Your healthcare team can help you build a comprehensive plan tailored to your specific needs. Physical therapy is more than pain relief—it's a whole‑body approach to movement, strength, and long‑term joint protection.
Improves joint function and flexibility
Gentle stretching and mobility exercises help increase range of motion, reduce stiffness, and make everyday movements more comfortable. Regular flexibility work also supports injury prevention and overall physical function. These activities should be performed gradually and safely, especially for individuals with existing joint or mobility challenges.
Improves muscular strength
Building muscle strength is essential for joint stability. Stronger muscles absorb more load, reducing stress on inflamed joints and lowering the risk of injury. Strength training supports better posture, balance, and long‑term joint health—key benefits for anyone managing autoimmune arthritis.
Improves balance and coordination
Consistent physical activity enhances balance and coordination, reducing the risk of falls—a common concern for those with autoimmune arthritis. Activities such as yoga, tai chi, Pilates, and targeted balance training help improve stability while supporting overall well‑being.
Manages pain and promotes relaxation
Physical therapists teach evidence‑based pain‑relief techniques, including heat therapy to improve circulation and reduce stiffness, and manual therapy or gentle massage to ease muscle tension. These approaches help calm irritated tissues and support relaxation.
Boosts mood and releases endorphins
Regular movement increases energy levels and supports emotional well‑being. Exercise triggers the release of endorphins—your body’s natural mood enhancers—helping you feel more positive, resilient, and energized.
What exercises will I do in physical therapy?
Your physical therapist will design a personalized program based on your symptoms, mobility, and goals. Most plans include a mix of strengthening, stretching, balance work, and low‑impact cardiovascular exercise.
Low‑impact cardio
Activities such as walking, cycling, or aquatic exercise help improve endurance without placing excessive stress on sensitive joints.
Low-impact cardiovascular exercises are an excellent way to support heart health and reduce inflammation. Activities such as walking, swimming, and cycling strengthen the cardiovascular system while lowering the risk of chronic illness. Incorporating these gentle, joint-friendly movements into your routine promotes overall wellness and supports long-term health.
Strength training
Strength training includes exercises that build muscle strength and increase muscle mass. By targeting the muscles surrounding your joints, this training improves support and stability, reduces injury risk, and enhances overall physical performance. Additional benefits include improved bone density, a more efficient metabolism, and greater functional strength for daily activities.
Range-of-motion exercises
Range-of-motion exercises help maintain flexibility and reduce joint stiffness. These movements guide your joints through their full motion, supporting mobility and function. When practiced consistently, they improve circulation and lower the risk of injury, making them a valuable part of any arthritis-friendly routine.
Balance and coordination exercises
Balance and coordination exercises strengthen stabilizing muscles and improve proprioception—your body’s ability to sense its position in space. Examples include standing on one leg, heel-to-toe walking, or using stability balls and balance boards. These exercises reduce fall risk, enhance agility, and improve overall body control.
How often should I go to physical therapy?
Your therapist will determine the ideal frequency of your sessions based on your needs and progress. Many people begin with 2–3 sessions per week for close guidance and support. As you gain strength, confidence, and independence, your therapist may transition you to weekly visits.
Over time, sessions may be spaced to every two weeks or once a month. This flexible schedule ensures you receive professional support while gradually taking more ownership of your home exercise program.
Is physical therapy safe for me with autoimmune arthritis?
Yes—physical therapy is not only safe but often essential for managing autoimmune arthritis. Therapists tailor exercises to your abilities, prioritize joint protection, and adjust your plan during flare-ups. Their goal is to help you move comfortably, safely, and confidently.
Your program will emphasize gentle range-of-motion work, gradual strengthening, and strategies that reduce strain on inflamed joints. Physical therapy becomes a powerful partner in reclaiming mobility and managing symptoms.
How can I find a good physical therapist for my autoimmune arthritis?
Finding the right therapist can feel overwhelming, but a few simple steps can guide you toward the best match for your needs.
Start with your doctor’s network
Your doctor may already work with trusted therapists who understand autoimmune arthritis. Their recommendations offer insight into a therapist’s expertise and approach.
Dive into online resources
Tools like the American Physical Therapy Association’s “Find a PT” directory allow you to filter by location, specialty, and certifications. You can also contact clinics directly to ask about their experience with autoimmune arthritis.
Seek out a personalized touch
Online reviews and personal recommendations from others with autoimmune arthritis can be invaluable. Look for therapists praised for empathy, communication, and condition-specific knowledge.
Trust your gut
A brief consultation helps you gauge a therapist’s communication style, understanding of your needs, and overall rapport. Choose the professional who makes you feel supported and confident in your journey.
In conclusion
Physical therapy is more than a treatment—it’s an investment in your future. It opens the door to reduced pain, improved movement, and renewed confidence. With the guidance of a skilled therapist, you can build personalized exercise routines, learn effective pain management strategies, and regain control of your mobility.
A small amount of dedication today can create a brighter, more active tomorrow. Physical therapy helps you reclaim your life, one movement at a time.
Physical Therapy and Autoimmune Arthritis: Detailed FAQ
Is gentle strength training safe during an autoimmune arthritis flare?
In many cases, yes—but it must be modified. During a flare, physical therapists often reduce resistance, shorten session length, and focus on pain-free range-of-motion and isometric exercises. The goal is to maintain joint support without provoking more inflammation. Always follow your therapist’s guidance and stop if pain sharply increases.
Can low-impact cardio reduce morning stiffness from autoimmune arthritis?
Short bouts of low-impact cardio, such as slow walking or gentle cycling, can improve circulation and help reduce morning stiffness. Many patients benefit from a brief warm-up routine recommended by their physical therapist, followed by stretching tailored to their joint limitations.
How do physical therapists adapt exercises for autoimmune arthritis fatigue?
Therapists use pacing strategies, shorter sets, longer rest breaks, and alternating muscle groups to respect fatigue. They may also recommend energy-conservation techniques for daily tasks, helping you stay active without overloading your joints or nervous system.
What should I tell my physical therapist before starting an autoimmune arthritis program?
Share your diagnosis, medications, recent flares, pain patterns, and any activities that worsen or relieve symptoms. Mention fatigue levels, sleep quality, and mobility challenges at home. The more specific you are, the more precisely your therapist can tailor your plan.
Physical therapy for autoimmune arthritis focuses on joint protection, low-impact exercise, flare-aware pacing, and individualized plans that integrate strength, flexibility, balance, and pain management. This FAQ targets nuanced, low-search-volume questions patients ask about safety, flares, fatigue, and communication with their care team.
📘 Related Patient Resources
The Log: Start tracking your "Mental Clarity" score with my Daily Glucose Tracker .
The Foundation: New to this? Read my Beginner’s Guide to Diabetes .
Liver Health: How metabolic syndrome impacts liver cirrhosis .
Fact-checking Sources
American Physical Therapy Association (APTA): https://www.apta.org/
Arthritis Foundation: https://www.arthritis.org/
Mayo Clinic: https://www.mayoclinic.org/


